There are many types of headache. You can read about them at the website of the International Headache Society.
The two commonest types of headache in neurological practice are migraine and ‘tension type’ headache. Many people have both types of headache as having one makes you more likely to have the other.
Most people with chronic headache have at least some migraine. The video below is a good introduction to migraine.
Tension type headache is misnamed because many patients with it are not stressed or tense. We also know that the problem is not just to do with tension of the muscles of the scalp.
I have included a page on headache here mainly to describe ‘Chronic Daily Headache’. This can arise out of migraine or tension type headache and is quite common in people with other functional neurological symptoms. You can download the factsheet on the right.
Chronic Daily Headache is the commonest type of headache that is referred to a neurology clinic.It refers to a headache that is present most days, often for most of the day. Typically it has the following features:
• Constant ‘pressing’ or ‘bursting’ sensation, sometimes pounding
• Can be all over head, on one side or sometimes in a small area
• It is often variable but tends to get worse as the day goes on
• Conventional painkillers only ‘take the edge’ off the pain
It is hard for others to understand how a headache can be so bad without any obvious cause other symptoms associated with Chronic Daily Headache

Often headache is not the only symptom that people with Chronic Daily Headache have. Below are some common symptoms that can go along with chronic daily headache.
• Fatigue / Tiredness
• Back or Neck pain
• Poor concentration
• Sleep disturbance (not enough or too much)
• Word finding difficulty
• Blurred vision
• Nausea
• Avoidance of bright light
• Frustration, Anger
• Low mood
• Lack of enjoyment
• Worry
It is true that Chronic Daily Headache is not a very glamorous sounding diagnosis. But it is widely recognised one in neurology and by the International Headache Society. It can arise out of both migraine or tension type headache. The name often doesn’t do justice to the severity of the pain.
Chronic daily headache is a very distinctive clinical condition. Just as neurologists don’t do a brain scan to diagnose migraine, it is usually not necessary to have a brain scan to diagnose chronic daily headache. This is particularly true if the headache has been going on for a few months.
Your doctor will have taken a careful history and performed a relevant examination. If they do not arrange a scan it is because they are confident about the diagnosis. They should have reassured you that there is not a sinister cause like a brain tumour.
Chronic Daily Headache is a complex phenomenon that probably has lots of different causes. Try thinking of the problem as a volume knob in your head that has been turned up too high.
As we understand more about the way pain works we know that there really are places in the nervous system, both in the nerve endings in the head and in the brain itself where this process of sensitisation and amplification of pain can occur. Try thinking of the problem as a volume knob in your head which has been turned up too high and which you need to turn down
These are some potentially relevant factors:
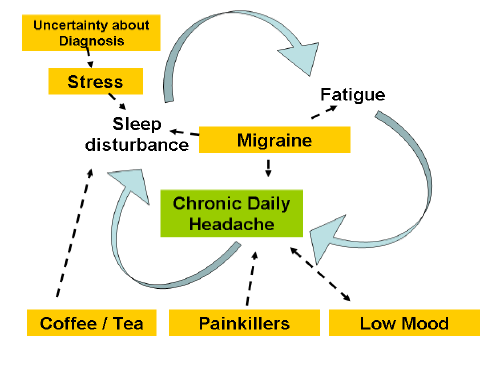
After a while many patients with chronic daily headache find they are in a vicious circle of symptoms (see picture on right)
If you have had the headache for a long time it will take a long time to improve. These things may help:
• Feeling satisfied with the diagnosis. If you have ongoing doubts that the diagnosis is wrong then it will be hard to get better.
• If you have migraine, then treatment of the underlying migraine can help a lot. Find out more about migraine from the Migraine Trust (UK) or the American Migraine Foundation (US)
• Stop regular analgesics. Try as hard as you can to stop taking all regular painkillers. This includes ibuprofen, paracetamol and codeine. When you stop them your headache will normally get temporarily worse (for several weeks) before it improves. There are two ways of stopping the tablets. Either set a date to stop them (like stopping smoking) or gradually wean yourself off them.
• Improve your sleep habits. Go to bed at the same time every night. Avoid coffee, tea or coca cola after 6pm. Is your bed comfortable / too hot / cold?
• Drug treatment—so-called antidepressants such as amitryptiline can be helpful in these illnesses, even for people who are not feeling depressed. They are used in migraine and back pain as well. They are not addictive, like Valium or codeine. They work by promoting sleep and helping to chemically ‘turn down’ the ‘volume knob’. You can get better without them
but they may well increase your chances of success. When you first start them you may experience side effects which should settle after a couple of weeks
• Look at stress/worry/mood. If you are under stress or feeling down for other reasons then finding ways to solve this may also improve your headache
• Other treatments. Neck physiotherapy may sometimes be offered. Alternative treatments such as acupuncture and massage are unproven but can help some patients.
Find out more about migraine and headache from the Migraine Trust (UK) or the American Migraine Foundation (US)
Lifestyle factors in Migraine
I particularly recommend the site Headache Relief Guide (www.headachereliefguide.com). This site made by Dr Jennifer Bickel and Dr Mark Connelly, paediatric neurologists in Kansas was designed for children and teenagers to give advice about modifiable lifestyle factors like exercise, sleep, hydration and diet. I think its really helpful for people with migraine and headache of any age.

Some people have migraine WITH aura, some WITHOUT aura.
Migraine aura happens when parts of the brain shut down during a migraine. A wave of overactivity mixed with underactivity sweeps through the brain, often from back to front.
The commonest migraine aura is VISUAL aura which comes from the back of the brain where the visual cortex lives. The video below is a really nice demonstration of what migraine visual aura looks like. It usually develops more slowly than is shown here.


We will be re-directing you to the University of Edinburgh’s donate page, which enable donations in a secure manner on our behalf. We use donations for keeping the site running and further FND research.
